Family Medicine – Curriculum
Family Medicine
Spokane Training Track
Our commitment to our residents is to provide a comprehensive educational experience. We remain committed to this mission and have adapted our curriculum to prepare our graduates for not only the cognitive, but also the procedural demands of the well-trained contemporary family physician.
First Year:
- Intro to Family Medicine (4 weeks)
- Outpatient Pediatrics and Specialty clinics (4 weeks)
- Adult Emergency Medicine + Clinic (4 weeks)
- Pediatric Emergency Medicine + Clinic (2 weeks Peds ER / 2 weeks clinic)
- Family Medicine Hospital Service (8 weeks)
- House Staff with Internal Medicine Residency (4 weeks)
- Inpatient Pediatrics (8 weeks)
- Gynecology + Clinic (4 weeks)
- Obstetrics (8 weeks)
- ICU (4 weeks)
Third Year:
- Outpatient Pediatrics and Specialty Clinics (4 weeks)
- Electives (12-16 weeks)
- Family Medicine Outpatient (8 weeks)
- Family Medicine Hospital Service (8 weeks)
- Obstetrics (4-8 weeks)
- Orthopedics/Sports Medicine (4 weeks)
- Geriatrics (4 weeks)
- Gynecology + Clinic (4 weeks)

Second Year:
- Outpatient Cardiology (4 weeks)
- Adult Emergency Medicine (4 weeks)
- Family Medicine Outpatient (4 weeks)
- Family Medicine Hospital Services (8 weeks)
- Inpatient Pediatrics (4 weeks)
- Obstetrics (4 weeks)
- Orthopedics/Sports Medicines (4 weeks)
- Rural Clerkship (4 weeks)
- Outpatient Pulmonology (4 weeks)
- Surgery + Clinic (4 weeks)
- Elective (4-8 weeks)

Introduction To Family Medicine
(Only for First-Year Residents)
This is the first four-week block of residency for all interns. During this block, residents will experience working in the Spokane Teaching Health Clinic, inpatient medicine service, and the obstetrical service. The goal is to familiarize each intern with a few core rotations and introduce one to working with the EMR (Epic). At STHC, they will begin to learn the interdisciplinary workflow while establishing relationships with their patient panel and become familiar with clinic policies and procedures. On inpatient medicine, while providing care for a limited number of patients, they will learn logistics of the hospital workflow such as how to do an admission or discharge at Sacred Heart Medical Center. On Labor and Delivery, they will observe the unique needs of laboring, postpartum, and antepartum patients. There is also time this block dedicated to other programmatic trainings that walk one through how to apply fluoride varnish to teeth in a pediatric patient, place a fetal scalp electrode, provide time to complete the Neonatal Resuscitation Program, or learn about clinic resources such as those provided by social workers or our collaborative care team.
Family Medicine
In addition to Introduction to Family Medicine in the R1 year, there are several four-week block rotations in the R2 and R3 years focusing on the ambulatory care setting and simulating a full-time clinic practice. Residents will concentrate on their own continuity clinics while gaining additional experience in specialty clinics. They will have additional training in procedures including IUD placement and removal, Nexplanon placement and removal, musculoskeletal injections, colposcopy, circumcision, and skin lesion removal. Residents will be available for same-day appointments to further gain experience in acute patient complaints. During this rotation, home visits may also be scheduled. The schedule is Monday-Friday with standard business hours and no call.
Cardiology
Four weeks are spent working with local cardiologists in their outpatient clinics. Residents evaluate new patients and follow-up on prior consults. They have opportunities to observe and learn the interpretation of exercise and nuclear stress tests as well as echocardiograms. This serves a valuable opportunity for residents to hone their EKG interpretation skills. Through this rotation, residents gain a better understanding of acute and chronic cardiac conditions. The schedule is Monday-Friday with standard business hours and no call.
Emergency Medicine
Residents in their R1 year spend one month at Providence Sacred Heart Medical Center, a Level 2 Trauma Center that serves a large portion of the Inland Northwest. Residents complete 18 shifts divided between the pediatric and adult ERs, with one day per week of continuity patient care in the clinic. Second-year residents rotate at the nearby MultiCare Deaconess Hospital. There, residents complete 14 shifts in the adult ER with one day per week in clinic. During these rotations, residents learn how to stabilize acutely ill patients while gaining hands-on experience in procedures such as suturing, reducing fractures and dislocations, and intubations. The schedule is variable with the resident working several different shifts for varied experiences.
Electives
Elective time in the R2 and R3 years may be used to pursue a wide range of medical and surgical interests. Electives include a variety of subspecialty rotations such as dermatology, rheumatology, transgender medicine, prison medicine, street medicine, osteopathic manipulation, and sports medicine, to name a few. Electives can also be international rotations, additional rural rotations, additional inpatient rotations, and procedural rotations; new electives can be designed to help residents achieve their educational goals. Residents on the OB track use one month in each of their R2 and R3 years for additional OB training. For each non-OB elective, the resident spends half of their time in their continuity clinic and half at the elective. The schedule is variable but is generally Monday-Friday with standard business hours and no call.
General Surgery
For two weeks during their R1 year, residents work with general surgeons in the community and at Sacred Heart Medical Center or MultiCare Deaconess Hospital. The focus is on preoperative assessment and management of postsurgical patients, assisting in the OR, postoperative care, and outpatient surgical management. The schedule is variable but is generally Monday-Friday with standard business hours and no call.
Health Systems Management (HSM)
Residents learn about various models of care throughout their residency training. We have connections with community clinics to provide a wide range of experiences including care for unhoused, English as a second language, and Native American populations. This curriculum also includes 1:1 billing coaching, motivational interview training, leadership meetings, and group visit experience. Group visits are offered twice monthly to STHC patients interested in improving their wellness and offer an alternative way to provide care and education to patients.
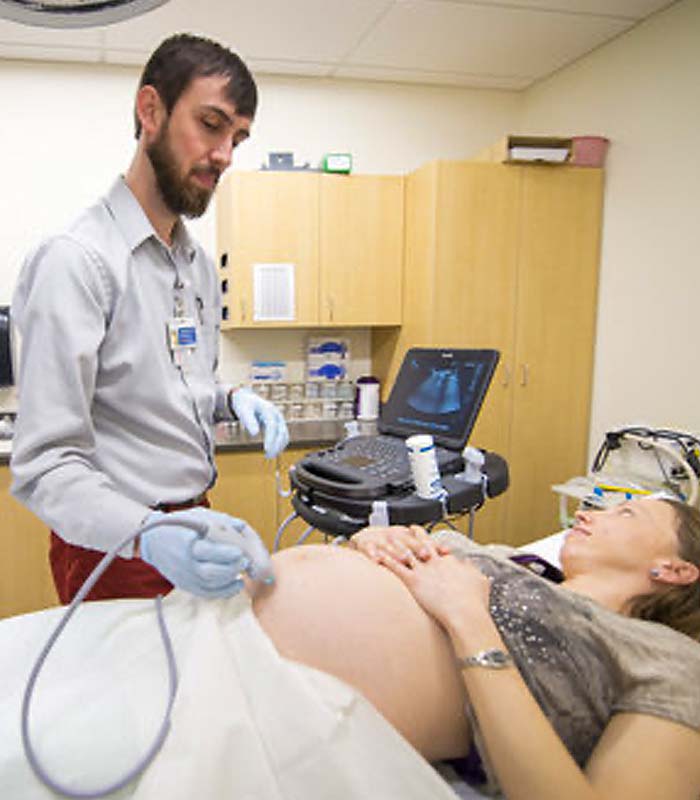
POCUS (Point-Of-Care Ultrasound)
Through a series of structured and longitudinal experiences, residents will have the opportunity to learn and perform POCUS in both the hospital and outpatient settings. Utilizing the program’s handheld portable ultrasound devices, residents can obtain and implement real time data while on rounds, in the STHC clinic or on the L&D floor. FMRS also has a state of the art ultrasound machine at the STHC for even higher tech visualization which residents will become familiar with throughout their sports medicine rotations.
Procedures
Residents have the opportunity to learn and perform common outpatient procedures during their Family Medicine clinic time during all 3 years of their residency. Augmented by lectures, residents can hone their procedural skills by performing common clinic procedures including skin biopsies, excisions, incision and drainage of abscesses, toenail removals, and wound care, joint injections, neonatal male circumcisions, endometrial biopsies, colposcopy and Long-Acting Reversible Contraception placement and removal, to name a few.
Gynecology
Gynecology and women’s health are taught as a combination of rotation time, longitudinal care, and online learning materials. The gynecology rotation occurs in two 2-week blocks, one in the first year and one in the third year of residency and is spent with local gynecologists and subspecialists. Residents also see gynecology patients in the continuity clinic and rural rotations and have ample opportunity to learn office gyn procedures including IUD’s, Nexplanon, endometrial biopsy, colposcopy and LEEP surgery.
Obstetrics
Residents rotate in obstetrics in all three years with an increasing level of responsibility. Interns are expected to complete two months of obstetrics. As seniors, they may choose to pursue an OB track, consisting of four months split between the R2 and R3 years. The minimum total OB requirement is four months. In addition to their own continuity patients, residents care for patients of community obstetricians and family physicians. Additionally, residents assist in caring for high risk patients of the OB hospitalists and perinatologists. Our OB fellowship serves to further support the experience. Call is shared either day or night on 12-hour shifts. All residents gain a robust experience in operative and non-operative obstetrics. Each resident is involved with approximately 60 to 80 deliveries per year.
Inpatient Adult Medicine
Our program has a very strong inpatient medicine curriculum. Residents will gain experience working with the family medicine and internal medicine inpatient teams. The family medicine panel is mainly led by family medicine trained faculty. The panel admits our clinic patients from STHC as well as general admissions to keep a consistent census. There are two interns and two seniors during the day with one senior resident covering at night. Patients offer a range of complexity. We have a nurse coordinator for discharge planning.
Inpatient and Outpatient Pediatrics
Inpatient Pediatrics training takes place at Sacred Heart Children’s Hospital, which serves as the pediatric referral center for the Inland Northwest. Residents work directly with pediatric hospitalists for 8 weeks during their intern year and 4 weeks during their R2 year. The pediatrics’ team is composed primarily of family medicine residents. In addition to daily teaching rounds, didactics are provided during the rotation. Family medicine residents typically have one full day of continuity clinic each week. Each resident on the team will typically provide night coverage for 5-6 nights during each rotation. Outpatient pediatric experience is provided through pediatric clinic visits during the resident’s continuity clinic as well as 8 weeks of dedicated outpatient pediatric experience, 4 weeks each during the intern and R3 year. Time is dedicated to general outpatient pediatrics, with an emphasis on newborn rounding, developmental assessment, adolescent medicine, eating disorders, ADHD and learning disabilities.
Rural Clerkship
A core element of the mission of Family Medicine Residency Spokane is to prepare graduates for practice in a broad range of clinical settings and locales. The key benefits of requiring a rural training experience at our Colville Rural Training Track sites are to expose the resident physician to the unique demands and advantages of practice within rural communities as family physicians. Our rural training sites expose our residents to role modeling by Family Physicians who provide not only an extensive range of primary, secondary emergency care, procedure and obstetrical skills, but also unique roles for involvement in the community and medical systems which are unique to rural practice. During their R2 year, residents will spend a 4 week rotation at our Colville RTT site in Colville, WA, where they will gain experience in rural hospital medicine, emergency medicine, obstetrics, and outpatient medicine. There will also be ample opportunities to hone their procedural skills, performing clinic procedures that are a part of the typical clinic day of a rural family doctor. The schedule is variable with the resident working several different shifts for varied experiences.
Musculoskeletal
Supervised by primary care sports medicine physicians and orthopedic physicians, residents will gain experience in evaluation and management of common musculoskeletal conditions, fracture care, pediatric musculoskeletal issues, as well as exposure to physical therapy. Opportunities for pre-participation exams and high school side-line sports medicine exist as well.
Didactics
Thursday afternoons are a dedicated time that runs an 18-month curriculum where residents, attendings, and guests provide educational seminars covering key topics in family medicine. This structure allows residents who may have missed a topic an opportunity to experience it and other residents to revisit the topic. Some Thursdays have devoted space for resident/faculty meetings and Graduate Medical Education all resident meetings and seminars. Attendance is required unless a resident is covering an inpatient service or scheduled off that day.
Osteopathic Principles and Practice
All residents learn the basic concepts of Osteopathic Manipulative Medicine to the extent of knowing good candidates for Osteopathic Manipulative Therapy and how to refer a patient for these services. Osteopathic trained (D.O.) residents who decide to continue to advance their skills for future practice will have clinical experiences for OMT throughout residency in their outpatient continuity clinic and the residency OMT clinic. Residents can advance their skills in hospitalized patients and provide OMT to patients on our medicine and obstetric/newborn services or have elective time dedicated to skill development. Residents apply their osteopathic principles and practice to their didactic lectures as appropriate and have opportunities to participate in Journal Club articles with other residencies.
Contact Us

Diane Borgwardt
Program Coordinator
Family Medicine Residency
Rural Training Track Residency
Sports Medicine Fellowship
OB Fellowship
624 E. Front Avenue
Spokane, WA 99202
Phone: 509-626-9900
